

Paradigm Shift Intervention Monitoring
 twitter
twitter

Commentary
Novel
Beta Coronavirus HCW Clusters Raise Concerns
Recombinomics
Commentary 19:00
December 3, 2012
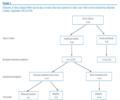
Figure 2. Outcome of close contact follow-up
ten days or more since last exposure to index case with a novel
coronavirus infection, London, September 2012 (n=64)
The above figure is from the Eurosurveillance
report entitled “The United Kingdom public health response to an
imported laboratory confirmed case of a novel coronavirus in September
2012” which included testing of contacts of the first confirmed novel
betacornavirus case (49M) from Qatar. As seen in the flow chart,
there were 13 health care worker (HCW) contacts who were
symptomatic. Ten were tested by PCR, but as noted above, samples
were collected from cases who were exposed 10 or more days prior to
collection. These HCWs were not hospitalized (they self
quarantined at home) and viral RNA levels would likely be low.
Thus, collection times would have to be optimal for detection, so a
failure to detect the novel betacornavirus was not unexpected.
Moreover, a fatal case (from Saudi Arabia), who died at the beginning
of September, was not tested.
The large frequency of
contacts with symptoms (13/56 = 23%) was similar to frequencies seen in
the SARS CoV outbreak in 2003, raising concerns that the negative data
for the HCWs reported above was false.
The cluster
in Jordan was more serious. The cases were linked directly or
indirectly to the ICU in Zarpa. Local media reports noted that
the presentation was similar to SARS and the symptomatic cases were
hospitalized. Although many of the 12 cases were only
hospitalized briefly, two of the cases died, one with renal
complications and the other with cardiac problems (which were in
addition to respiratory problems). Samples were sent to labs in
France and Egypt. The ECDC
report noted that the US CDC and WHO were aware of the
outbreak. Initial testing in April was negative for respiratory
virus including a panel of known coronaviruses, including SARS.
However re-testing use a PCR test using the sequence from the initial
isolate, EMC/12, identified the virus in the two fatal cases.
The positive results were reported by
WHO, but the report had no detail (age, gender, or key dates of
disease onset, hospitalization, death or discharge). However,
media reports on the press conference by the Jordan MoH indicated the
first fatality (40F nurse) died on April 19, while the second fatality
(25M intern) died on April 26. The one week gap in date of
death suggests that disease onset dates had gaps supporting human to
human (H2H) transmission, as did symptoms in the son of the first fatal
case.
The confirmation of the novel
coronavirus in two members of the cluster, as well as symptoms in at
least one family member and the 1 week gap in the date of death for the
two fatal cases, raises strong concerns that the other members of the
cluster were also infected, but tested negative due to collection
and/or sensitivity issues.
The transmission within the
group is also supported by the Riyadh family cluster, which tested
positive for three of the four symptomatic family members, including
the two fatal cases whose
date of death were at least 4 days apart.
Although WHO undoubtedly has
the age, gender, and key dates for each of the confirmed / probable /
suspect cases in these clusters, the data has been withheld as WHO
continues to cite possible common sources for the clusters, which have
no scientific support, but are cited, in part, because the data that
contradicts this possibility is withheld.
WHO should release the
withheld data, which will strongly support sustained human transmission
over a seven month period. Sequences should also be released,
which will also clearly support the emergence of a human contagion.
Recombinomics
Presentations
Recombinomics
Publications
Recombinomics
Paper
at Nature Precedings